Cortisol
Obesity and type 2 diabetes are metabolic problems caused by too much cortisol.
Before my heart attack, I believed that we could prevent obesity, diabetes, and heart disease by eating less and exercising more. I was wrong. These disorders are caused by the inflammation and cortisol we produce to fight infections. Diet and exercise have some effect on them, but not much.
Stress produces extra cortisol and contributes to our health problems, as shown below.
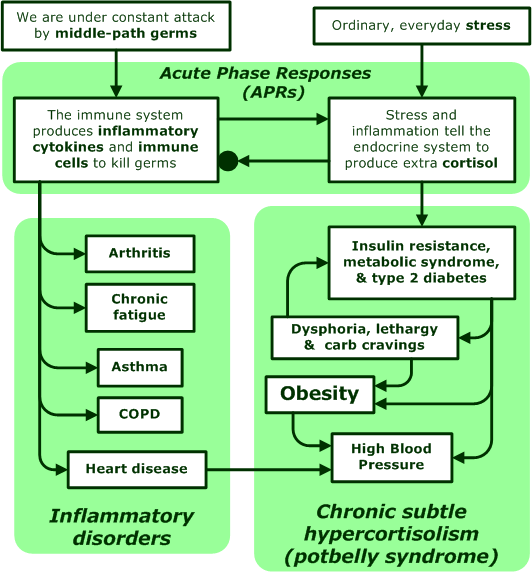
Cortisol-related health problems
When we are under stress, or have an infection, cortisol raises our blood pressure and blood sugar levels. These changes help us survive short periods of stress, but they hurt us when they continue for years and years. The symptoms of long-term, moderately high cortisol (chronic subtle hypercortisolism) include:
- Suppressed immunity, leading to more infections
- High blood pressure (hypertension)
- High blood sugar (hyperglycemia)
- Insulin resistance and dysphoria that lead to carbohydrate cravings, metabolic syndrome, obesity, and type 2 diabetes
- Fat deposits on the face, neck, and belly
- Reduced libido
- Suppressed thyroid hormones
Cushing's syndrome. High levels of cortisol cause a serious disease called Cushing's Syndrome, which is sometimes called hypercortisolism. Insulin resistance, metabolic syndrome, and diabetes are common, and most people with untreated Cushing's syndrome will die from heart disease. (See Cushing's Syndrome link at left.)
Potbelly syndrome. The technical name for potbelly syndrome is chronic subtle hypercortisolism, and it is an extension of the metabolic syndrome. PubMed lists 25,000+ studies that mention metabolic syndrome.
Cortisol and inflammation
Cortisol is a powerful anti-inflammatory hormone, so you might think that high levels of it would protect us from inflammatory diseases like arthritis and heart disease. Unfortunately, it doesn't.
Cortisol and cortisol-like medicines suppress inflammation by suppressing parts of the immune system. That makes us more susceptible to new infections, and sooner or later we will get them. The new infections will raise our inflammation and cortisol levels, making us susceptible to still more infections. And so on.
Because of this "bootstrapping" effect, cortisol tends to make inflammatory illnesses worse over a long period of time. Cortisol may help with problem X, but it is likely to make problem Y worse.
Stress makes the bootstrapping effect worse, and sometimes just reducing stress will do wonders for our health. Unfortunately, stress reduction is not an easy or reliable method of dealing with chronic infections.
Summary
A healthy lifestyle, with exercise, rest, vitamins, and a good diet, can slow down the processes described above and lower cortisol levels. A healthy lifestyle cannot prevent or cure obesity, diabetes, or heart disease because it cannot kill the germs that cause them.
More information on cortisol
Acute phase responses are discussed in Chapters 2 and 3 of The Potbelly Syndrome.
HPA Axis. Cortisol is produced and regulated by the hypothalamic-pituitary-adrenal (HPA) axis. A large part of The Potbelly Syndrome, especially Chapter 15, is devoted to discussions of cortisol and the HPA axis. There are pretty good descriptions of cortisol and the HPA axis at:
Cortisol and addiction. Cortisol has been linked to a number of addictive substances, so the U.S. National Institute on Alcohol Abuse and Alcoholism (http:⁄⁄www.niaaa.nih.gov) has an interest in it. The articles listed below give excellent descriptions of how cortisol is produced, and what its effects are. The articles are pretty technical, but they are well written and fairly easy to read.
- Stress primer: http:⁄⁄pubs.niaaa.nih.gov⁄publications⁄arh23-4⁄241-249.pdf
- Stress responses: http:⁄⁄pubs.niaaa.nih.gov⁄publications⁄arh22-1⁄67-72.pdf
- Alcohol-seeking:http:⁄⁄pubs.niaaa.nih.gov⁄publications⁄arh22-3⁄202.pdf
- Aging and stress: http:⁄⁄pubs.niaaa.nih.gov⁄publications⁄arh23-4⁄272-283.pdf
- The endocrine system: http:⁄⁄pubs.niaaa.nih.gov⁄publications⁄arh22-3⁄153.pdf
- Immune suppression: Immune Suppression
Torpy DJ, Ho JT. Value of free cortisol measurement in systemic infection. Horm Metab Res. 2007 Jun;39(6):439-44. Review.
Miyashita N. [Chlamydia pneumoniae infections] Kekkaku. 2006 Sep;81(9):581-8. Review. Japanese.
Rotman-Pikielny P, Roash V, Chen O, Limor R, Stern N, Gur HG. Serum cortisol levels in patients admitted to the department of medicine: Prognostic correlations and effects of age, infection, and comorbidity. Am J Med Sci. 2006 Aug;332(2):61-7.
Manary MJ, Muglia LJ, Vogt SK, Yarasheski KE. Cortisol and its action on the glucocorticoid receptor in malnutrition and acute infection. Metabolism. 2006 Apr;55(4):550-4.
Bouyou-Akotet MK, Adegnika AA, Agnandji ST, Ngou-Milama E, Kombila M, Kremsner PG, Mavoungou E. Cortisol and susceptibility to malaria during pregnancy. Microbes Infect. 2005 Aug-Sep;7(11-12):1217-23.
Huitinga I, Erkut ZA, van Beurden D, Swaab DF. The hypothalamo-pituitary-adrenal axis in multiple sclerosis. Ann N Y Acad Sci. 2003 May;992:118-28. Review.
